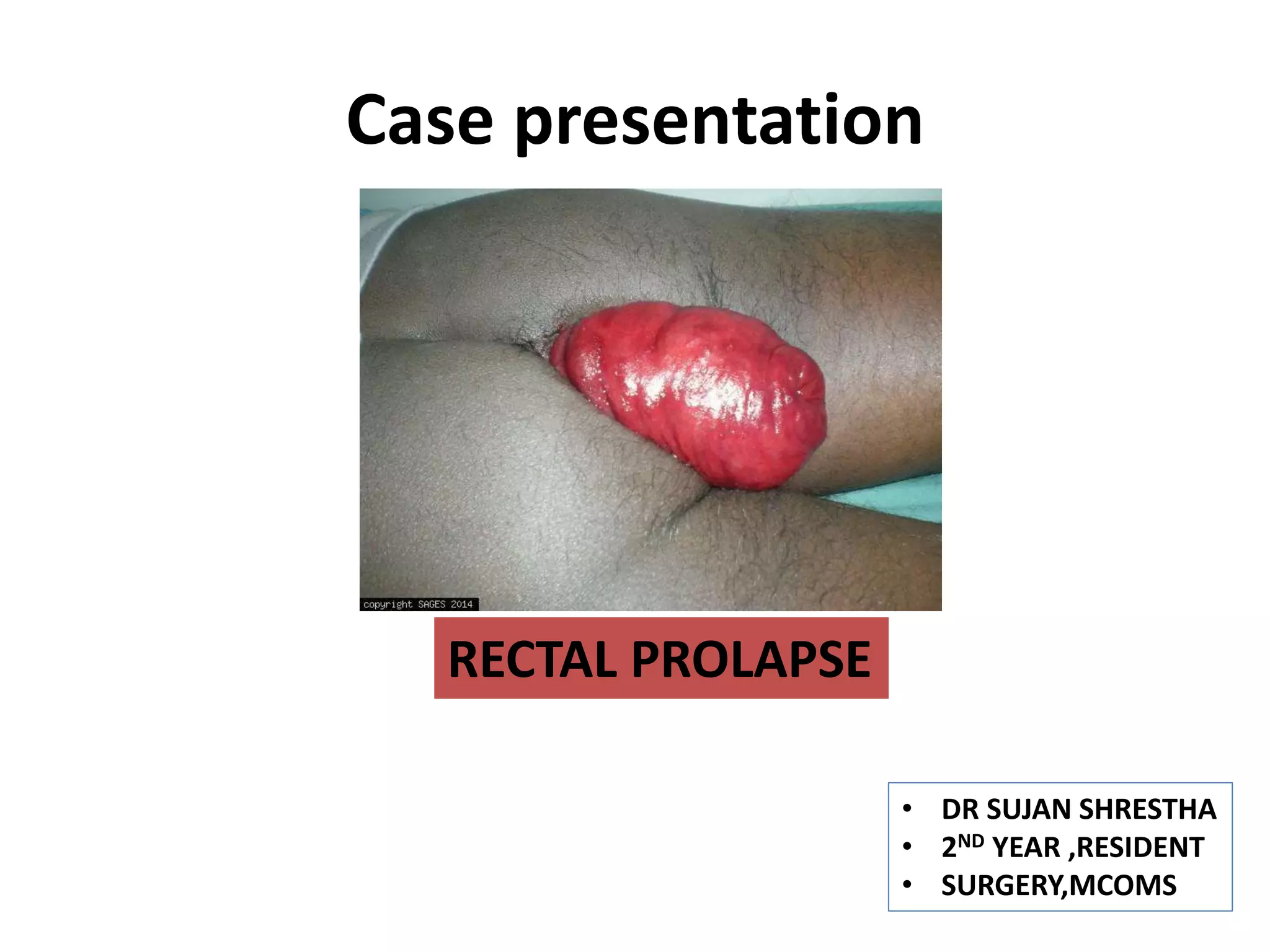
Anal prolapse is a condition that occurs when the rectum protrudes through the anus, often due to weakened pelvic floor muscles or other underlying issues. This condition can be distressing and uncomfortable, and it is essential to understand its causes, symptoms, and treatment options. One of the critical aspects of diagnosing and treating anal prolapse is the use of images of anal prolapse, which provide valuable insights into the severity and nature of the condition.
Understanding Anal Prolapse
Anal prolapse, also known as rectal prolapse, is a medical condition where the rectum, the final section of the large intestine, protrudes through the anus. This condition can be partial or complete, depending on the extent of the prolapse. Partial prolapse occurs when only the inner lining of the rectum protrudes, while complete prolapse involves the full thickness of the rectal wall.
Anal prolapse can affect individuals of all ages but is more common in older adults, particularly women. The condition is often associated with weakened pelvic floor muscles, which can result from childbirth, chronic constipation, or other factors that put pressure on the pelvic area.
Causes of Anal Prolapse
The primary causes of anal prolapse include:
- Weakened Pelvic Floor Muscles: Childbirth, especially vaginal deliveries, can weaken the pelvic floor muscles, making them less effective in supporting the rectum.
- Chronic Constipation: Straining during bowel movements can put excessive pressure on the pelvic floor, leading to prolapse.
- Aging: As people age, the muscles and tissues in the pelvic area can weaken, increasing the risk of prolapse.
- Neurological Conditions: Conditions that affect nerve function, such as multiple sclerosis or spinal cord injuries, can also contribute to anal prolapse.
- Previous Surgeries: Previous pelvic surgeries can weaken the supporting tissues, making prolapse more likely.
Symptoms of Anal Prolapse
The symptoms of anal prolapse can vary depending on the severity of the condition. Common symptoms include:
- Rectal Bleeding: Blood may be noticed on toilet paper or in the stool.
- Mucus Discharge: A clear or yellowish discharge from the rectum.
- Pain and Discomfort: Pain in the rectal area, especially during bowel movements.
- Feeling of Incomplete Emptying: A sensation that the bowel is not completely empty after a movement.
- Visible Prolapse: The rectum may be visible outside the anus, especially during bowel movements.
In some cases, anal prolapse may not cause any symptoms, and the condition is discovered during a routine medical examination.
Diagnosing Anal Prolapse
Diagnosing anal prolapse typically involves a combination of physical examination and imaging tests. Images of anal prolapse play a crucial role in the diagnostic process, providing detailed visual information about the extent and nature of the prolapse.
During a physical examination, the healthcare provider will:
- Inspect the anal area for any visible prolapse.
- Perform a digital rectal exam to assess the strength of the pelvic floor muscles and the presence of any abnormalities.
- Ask about symptoms and medical history to better understand the underlying causes.
Imaging tests, such as defecography and magnetic resonance imaging (MRI), are often used to obtain images of anal prolapse. These tests provide detailed visual information about the structure and function of the pelvic floor and rectum.
Defecography involves taking X-ray images of the pelvic area while the patient is having a bowel movement. This test can show how the rectum and pelvic floor muscles function during defecation and can help identify the extent of the prolapse.
MRI provides high-resolution images of the pelvic area, allowing healthcare providers to assess the soft tissues and muscles in detail. This test can help identify any underlying conditions that may be contributing to the prolapse.
Treatment Options for Anal Prolapse
The treatment for anal prolapse depends on the severity of the condition and the individual's overall health. Treatment options range from conservative measures to surgical interventions.
Conservative Treatment
For mild cases of anal prolapse, conservative treatment options may be sufficient. These include:
- Dietary Changes: Increasing fiber intake can help soften stools and reduce straining during bowel movements.
- Hydration: Drinking plenty of fluids can help prevent constipation and reduce the risk of prolapse.
- Pelvic Floor Exercises: Kegel exercises can help strengthen the pelvic floor muscles and improve their ability to support the rectum.
- Medications: Stool softeners or laxatives may be prescribed to help prevent constipation.
Surgical Treatment
For more severe cases of anal prolapse, surgery may be necessary. Surgical options include:
- Rectopexy: This procedure involves reattaching the rectum to the sacrum, the bone at the base of the spine, to provide additional support.
- Rectal Plication: This procedure involves folding and suturing the rectum to reduce its length and prevent prolapse.
- Perineal Rectosigmoidectomy: This procedure involves removing a portion of the rectum and sigmoid colon and reattaching the remaining rectum to the anus.
Images of anal prolapse obtained during diagnostic tests can help healthcare providers determine the most appropriate surgical approach based on the individual's specific condition.
📌 Note: Surgery for anal prolapse is typically performed under general anesthesia and may require a hospital stay. Recovery time can vary depending on the type of surgery and the individual's overall health.
Preventing Anal Prolapse
While not all cases of anal prolapse can be prevented, there are several steps individuals can take to reduce their risk:
- Maintain a Healthy Diet: Consuming a diet rich in fiber can help prevent constipation and reduce straining during bowel movements.
- Stay Hydrated: Drinking plenty of fluids can help keep stools soft and easy to pass.
- Exercise Regularly: Regular physical activity can help strengthen the pelvic floor muscles and improve overall health.
- Avoid Straining: Avoiding prolonged straining during bowel movements can help prevent damage to the pelvic floor muscles.
- Manage Chronic Conditions: Properly managing conditions such as diabetes or neurological disorders can help reduce the risk of anal prolapse.
Living with Anal Prolapse
Living with anal prolapse can be challenging, but with the right treatment and lifestyle changes, many individuals can manage their symptoms effectively. It is essential to work closely with healthcare providers to develop a personalized treatment plan that addresses the individual's specific needs and concerns.
Support groups and online communities can also provide valuable resources and emotional support for individuals living with anal prolapse. Sharing experiences and learning from others can help individuals feel less isolated and more empowered to manage their condition.
Regular follow-up appointments with healthcare providers are crucial for monitoring the condition and adjusting treatment as needed. Early detection and intervention can help prevent complications and improve overall quality of life.
Images of anal prolapse obtained during diagnostic tests can provide valuable insights into the progression of the condition and the effectiveness of treatment. Regular imaging tests can help healthcare providers assess the need for additional interventions and make informed decisions about ongoing care.
In some cases, individuals may need to make lifestyle adjustments to accommodate their condition. This may include modifying dietary habits, engaging in regular exercise, and practicing good bowel habits. Working closely with healthcare providers can help individuals develop a comprehensive plan that addresses all aspects of their health and well-being.
It is essential to remember that anal prolapse is a manageable condition, and with the right treatment and support, individuals can lead fulfilling and active lives. Seeking medical attention early and following a personalized treatment plan can help individuals achieve the best possible outcomes and improve their overall quality of life.
In conclusion, anal prolapse is a condition that can significantly impact an individual’s quality of life. Understanding the causes, symptoms, and treatment options is crucial for effective management. Images of anal prolapse play a vital role in diagnosing and monitoring the condition, providing valuable insights into its severity and progression. With the right treatment and lifestyle changes, individuals can manage their symptoms effectively and lead fulfilling lives. Regular follow-up with healthcare providers and a proactive approach to care can help individuals achieve the best possible outcomes and improve their overall well-being.